Stomach Cancer / Gastric Cancer
If stomach cancer is diagnosed at an early stage, there is a good chance of a cure. In general, the more advanced the cancer (the more it has grown and spread), the less chance that treatment will be curative. However, treatment can often slow the progress of the cancer.
What is the stomach?
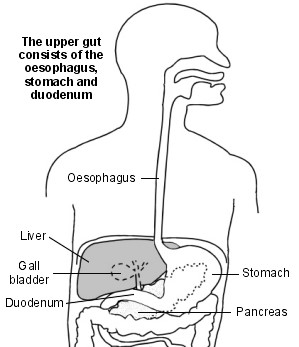
The upper gut
The stomach is in the upper tummy (abdomen). It is part of the gut (gastrointestinal tract). It lies in the upper part of the abdomen, just below the ribs. When we eat, food passes down the gullet (oesophagus) into the stomach.
The stomach makes acid and some chemicals (enzymes) which help to digest food. The muscles in the wall of the stomach tighten (contract) to mix up the food with the acid and enzymes.
Food then passes into the first part of the small intestine (the duodenum). Here food mixes with more enzymes which come from the pancreas and lining of the gut. The enzymes break down (digest) the food.
Digested food is then absorbed into the body from the small intestine.
What is stomach cancer?
Stomach cancer is sometimes called gastric cancer. Worldwide it is one of the most common cancers. It is common in Japan and China but is less common in the UK. About 5,000 people develop stomach cancer each year in the UK. Stomach cancer is more common in men than in women and tends to occur mainly in older people. Most people who develop stomach cancer are over the age of 55.
Adenocarcinoma of the stomach
In most cases, stomach cancer begins from a cell which is on the inside lining of the stomach (the mucosa). This type of stomach cancer is called adenocarcinoma of the stomach. As the cancer cells multiply:
- The tumour may invade deeper into the wall of the stomach. In time, it may pass through the wall of the stomach and invade nearby organs such as the pancreas or liver.
- The tumour may spread up or down the stomach into the gullet (oesophagus) or small intestine.
- Some cells may break off into the lymph channels or bloodstream. The cancer may then spread to nearby lymph nodes or spread to other areas of the body (metastasise).
Other types of stomach cancer
There are some less common and rare types of stomach cancer which include:
- Lymphomas. These are cancers which arise from the lymphatic tissue within the wall of the stomach.
- Sarcomas. These are cancers which arise from the muscle or connective tissue within the wall of the stomach.
- Carcinoid cancers. These are cancers which arise from cells in the stomach lining which make hormones.
The rest of this leaflet only discusses adenocarcinoma of the stomach.
What causes stomach cancer
A cancerous (malignant) tumour starts from one abnormal cell. The exact reason why a cell becomes cancerous is unclear. It is thought that something damages or alters certain genes in the cell. This makes the cell abnormal and multiply out of control. (See separate leaflet called Cancer for more details.) Many people develop stomach cancer for no apparent reason. However, certain risk factors increase the chance that stomach cancer may develop. These include:
- Ageing. Stomach cancer is more common in older people. Most cases are in people over the age of 55.
- Having a type of anaemia called pernicious anaemia, which causes a lack of vitamin B12, can very slightly increase your risk of stomach cancer.
- Diet is probably a factor:
- Countries such as Japan, where people eat a lot of salt, and pickled and smoked foods, have a high rate of stomach cancer.
- Eating a lot of fruit and green vegetables can reduce the risk.
Smokers have a higher rate of stomach cancer compared with people who do not smoke.
Long-term infection of the stomach lining with a germ (bacterium) called Helicobacter pylori (H. pylori) seems to lead to a slightly higher risk of stomach cancer. (This infection is very common in the UK, and most people with H. pylori infection do not develop stomach cancer.
Gender. Stomach cancer is twice as common in men as it is in women.
If you have had part of your stomach removed in the past for any reason. For example, to treat a stomach ulcer or some other condition.
Family history. For some cases, stomach cancer may run in the family. However, most cases of stomach cancer do not run in families and are not inherited.
Blood group A. People who have this blood group have a slightly higher risk.
Stomach cancer symptoms
When a stomach (gastric) cancer first develops and is small, it usually causes no symptoms. Some do not cause symptoms until they are quite advanced. Initial symptoms may include:
- Pain or discomfort in the upper tummy (abdomen), especially after eating.
- Indigestion. (Note: most people who have indigestion do not have stomach cancer.)
- Feeling sick, and being off food. Some people have a sense of fullness after eating.
- Weight loss and/or loss of appetite.
- You may pass blood out with your stools (faeces). This usually presents as black faeces (called melaena) or dark blood rather than bright red bleeding - which is more unusual with stomach cancer - and implies very serious bleeding in the stomach or bowel.
As the cancer grows in the stomach, symptoms may become worse and may include:
- The same symptoms as above, but more severe.
- Feeling generally unwell and more tired than usual.
- Becoming anaemic if the tumour regularly bleeds. This can cause you to become more tired than usual.
- The cancer growing very large and causing a blockage to food and drink.
If the cancer spreads to other parts of the body, various other symptoms can develop.
Note: all the above symptoms can be due to other conditions, so tests are needed to confirm stomach cancer.
How is stomach cancer diagnosed and assessed?
Initial assessment and gastroscopy (endoscopy)
If a doctor suspects that you may have stomach (gastric) cancer, he or she may examine you. The examination is often normal, especially if the cancer is at an early stage. Therefore, a gastroscopy is usually arranged. A gastroscope (endoscope) is a thin, flexible, telescope. It is passed through the mouth, into the gullet (oesophagus) and down towards the stomach and the first part of the small intestine (the duodenum). The endoscope contains fibre-optic channels which allow light to shine down so the doctor or nurse can see inside your stomach and duodenum.
Biopsy - to confirm the diagnosis
When a small sample of tissue is removed from a part of the body, the procedure is called a biopsy. The sample is then examined under the microscope to look for abnormal cells. When you have a gastroscopy, if anything abnormal is seen, the doctor or nurse can take a biopsy. This is done by passing a thin grabbing instrument down a side channel of the gastroscope. It can take two weeks for the biopsy results.
Assessing the extent and spread
If you are confirmed to have stomach cancer, further tests may be done to assess if it has spread. For example, a barium meal X-ray, a computerised tomography (CT) scan, a magnetic resonance imaging (MRI) scan, an ultrasound scan, laparoscopy or other tests. This assessment is called staging of the cancer.
The aim of staging is to find out:
- How much the tumour in the stomach has grown, and whether it has grown partially or fully through the wall of the stomach.
- Whether the cancer has spread to local lymph nodes.
- Whether the cancer has spread to other areas of the body (metastasised).
By finding out the stage of the cancer it helps doctors to advise on the best treatment options. It also gives a reasonable indication of outlook (prognosis). (See separate leaflet called Stages of Cancer for more details.)
Surgery
Removing the tumour may be curative if the cancer is in an early stage. The common operation is to cut out the affected part of the stomach. Sometimes the whole of the stomach is removed. Sometimes this is done laparoscopically (keyhole surgery). Even if the cancer is advanced and a cure is not possible, some surgical techniques may still have a place to ease symptoms. For example, a blockage may be eased by removing part of the stomach, or by using laser surgery or by a bypass operation.
Chemotherapy
Chemotherapy is a treatment of cancer by using anti-cancer medicines which kill cancer cells or stop them from multiplying. (See separate leaflet called Chemotherapy for more details.) When chemotherapy is used in addition to surgery it is known as adjuvant chemotherapy. For example, following surgery you may be given a course of chemotherapy. This aims to kill any cancer cells which may have spread away from the primary tumour. Sometimes, chemotherapy is given before surgery, to shrink a large tumour so that surgery is easier - this is known as neoadjuvant chemotherapy.